This website uses cookies as well as similar tools and technologies to understand visitors’ experiences. By continuing to use this website, you consent to Columbia University’s usage of cookies and similar technologies, in accordance with the Columbia University Website Cookie Notice.
Guest
Dr. Renee Salas
Center for Climate, Health, and the Global Environment at Harvard’s T.H. Chan School of Public Health
Wildfires, extreme heat and particulate matter from fossil fuel power plants are increasingly affecting the well-being of people in the U.S. and other countries.
In this episode, host Bill Loveless visits with Dr. Renee Salas about the adverse impacts of climate change on public health. As a leading public health researcher and emergency medical doctor, Dr. Salas has published extensively and testified in Congress on the impact of climate change on healthcare and the medical system.
She served as the lead author of the Lancet Countdown on Health and Climate Change U.S. Brief since 2018.
Dr. Salas is a Yerby Fellow at the Center for Climate, Health, and the Global Environment at Harvard’s T.H. Chan School of Public Health. She is also a practicing emergency medical physician at Massachusetts General Hospital and an assistant professor of emergency medicine at Harvard Medical School.
They bring us a compelling conversation about the mindset shift necessary to address the climate health crisis head on.
Transcript
Renee Salas: [00:00:03] An emergency department, I focus on why the patient is primarily there, so it’s sort of the primary diagnosis. So in this patient’s case, she came in for an asthma attack, but yet there’s so many items that we consider a secondary diagnosis, and those are just diagnoses that make it harder for us to either prevent or manage that primary diagnosis and climate change is actually a missing diagnosis in this patient. [00:00:29][25.2]
Bill Loveless: [00:00:29] The impacts of climate change on public health are getting more attention, though, as doctors look closer at some of the underlying causes of their patients symptoms. Extreme heat, wildfires and other developments altering our environment all contribute to illnesses showing up in hospital emergency rooms and doctor’s offices. But even as a growing body of research tells us more about climate change and its adverse impacts on public health, questions remain. What more do we need to learn to better understand this intersection of climate and health? And how can governments craft policies that will form the building blocks for a climate conscious medical system? This is Columbia Energy Exchange, a weekly podcast from the Center on Global Energy Policy at Columbia University. I’m Bill Loveless. Today on the show, Dr Renee Salas, she’s a Irby fellow at the Center for Climate, Health and the Global Environment at Harvard University’s T.H. Chan School of Public Health. She is also a practicing emergency medical physician at Massachusetts General Hospital and an assistant professor of emergency medicine at Harvard Medical School. Among her other career achievements, Dr Salas has served as the lead author of The Lancet Countdown on Health and Climate Change U.S. Breathe since 2018 and leads its working group of more than 70 U.S. organizations, institutions and centers working at the nexus of climate change and health. Dr. Solis received her Doctor of Medicine and a Master of Science in clinical research from the Cleveland Clinic Lerner College of Medicine. She also earned a Master of Public Health from the Harvard T.H. Chan School of Public Health with a concentration in environmental health. We’re thrilled to have her on the show for an all too rare conversation on the intersection of public health policy and the climate crisis. Please enjoy Dr. Rene Salis. Welcome to Columbia Energy Exchange. [00:02:41][131.4]
Renee Salas: [00:02:42] Thank you. It’s an honor to be here. [00:02:43][1.5]
Bill Loveless: [00:02:44] Well, first, tell us a little bit about yourself. Why did you become a doctor? [00:02:49][4.9]
Renee Salas: [00:02:49] I loved science and I loved people, and I wanted to serve people, and I volunteered at a hospital in my hometown and fell in love with it, and I would have been on that journey ever since. And then I really especially felt called to emergency medicine because it allowed me to treat the breadth of my community. And I love being able to treat whoever it is that walks through the door for whatever it is they need at whatever hour. [00:03:16][26.9]
Bill Loveless: [00:03:17] Yeah, and we have such great appreciation these days for those of you doctors and nurses and others who work in emergency rooms, just giving the stress that all of you have been undergoing with COVID. So so thank you for your service and your work along those lines. You know, we’re here to talk about the effects of climate change on public health. And as an emergency room physician, you observe firsthand the effects of this changing climate on people’s health, perhaps in ways that are not immediately obvious to your patients or their families. Give us some examples of what you see. [00:03:53][35.7]
Renee Salas: [00:03:54] I’m going to start with a story about a four year old girl who presented for her third asthma attack that week. It was an overnight shift, and I’ll never forget the conversation that I had with her mother. And she looked at me with this worry in her eyes and said, I’m doing everything that doctors have told me to do, but yet she’s not getting better. What am I missing? And that very question is, is something that I have asked myself and continue to ask myself about. What is it that we’re missing? And at an emergency department, I focus on why the patient is primarily there. So it’s sort of the primary diagnosis. So in this patient’s case, she came in for an asthma attack. But yet there’s so many items that we consider a secondary diagnosis, and those are just diagnoses that make it harder for us to either prevent or manage that primary diagnosis and climate change is actually a missing diagnosis in this patient. And the reason behind that is that climate change is driving pollen levels to be 50 percent longer and about eight percent higher concentration, according to a recent study. And I often think about when I see patients that I’m standing on a river, pulling them out one at a time, only to see many more behind them. And so it’s so important to walk upstream to figure out what it is that’s causing patients to fall into the river in the first place. And I realize when we walk upstream, we find the burning of fossil fuels is driving air pollution, especially inequitable exposure to air pollution and also driving climate change. So then we see that connection on why those pollen levels matter and why climate change matters to my patient. And in addition, for this particular patient, she lived in an area that was very close to a highway and so was disproportionately exposed to high levels of air pollution. But when I make that diagnosis of climate change, I realize it needs a different toolbox. [00:05:57][123.3]
Bill Loveless: [00:05:58] Yeah, because you can say that, I guess you can express that to add this to this patient’s parent. But this there’s not a whole lot you can do beyond treating the immediate symptoms. [00:06:09][10.5]
Renee Salas: [00:06:10] In many ways, it’s like putting a Band-Aid on a bullet wound and that. But the importance of recognizing climate change as a diagnosis is that we can actually begin to develop what needs to be done, which shows why upstream action is so important in order to address. The health impacts that we see in our hospitals and in my emergency department rooms, [00:06:31][21.8]
Bill Loveless: [00:06:32] Renee has your training as a doctor prepared you, or perhaps it hasn’t didn’t prepare you for diagnosing some of these climate related ailments. [00:06:42][9.6]
Renee Salas: [00:06:43] We’re very good at diagnosing these downstream impacts. But once we think about climate change as a medical diagnosis and we’re very good at writing out treatment plan, so asthma attack, we want to give albuterol inhalers and steroid prescriptions. But then once we address this, these other issues, then we start to think about interventions like thinking about air filtration systems and houses, thinking about how to weatherize homes. So that way, patients can have at least one environment where the air is not worsening their underlying lung conditions. And then we also think about policy related to the types of energy we use and and climate change policy. And that once we start getting into these public health interventions and these type of policy related issues, that’s an area where we have not been as well trained in medicine. And I think there is a growing recognition that it is critically important in this day and age that if we really want to get to the root cause of health and equity, that we have to have this additional tools in our box [00:07:54][70.9]
Bill Loveless: [00:07:55] now and for several years now, you’ve studied some of these big changes in the climate that are affecting people’s health, like changes in pollen seasons, as you just alluded to with the story about one of your patients and as well as extreme weather and vector borne diseases. You talked a little bit about the pollen. Could you could explain some of these other changes that take that are taking place in our environment and the risks they pose to people’s health? [00:08:24][28.9]
Renee Salas: [00:08:25] Yeah. From my vantage point, we are the face of climate change because climate change is here and now and it’s already harming our health. And I would argue everyone’s health is impacted to some degree. And some people, it leads them to being hospitalized or even die, and for others, it could be a transient cough. And the way I think about it is really in the following way of thinking about exposure pathways for climate change. So we think about the fact that heat is becoming more intense. It’s lasting longer and it’s happening more frequently. And heat has significant implications for health, especially for people who have underlying medical conditions. So heat stroke is the most life threatening form of heat illness. It also has implications for pregnant women. It has issue implications for people with mental health conditions and has been associated with worsening those and especially putting people at risk who have are on medications that make it harder for them to be able to regulate their body temperature and heat. But then we move along the spectrum and there’s poor air quality. So thinking about wildfire smoke, which has traveled across the country or this ground level ozone, which is driven higher by heat, then we think about how it impacts our food and water. So food is actually and crops are less nutritious because of climate change, which is especially important for people on the nutritional margin. And if we think about water impacts, Vibrio is a bacteria that grows in saltwater. So any oyster lovers out there, people who like to swim in ocean water. We’ve actually found here in the Northeast that the conditions are becoming more suitable for this bacteria to grow. And that’s just one example of many. And you brought up vector borne diseases. And so how ticks and mosquitoes live in their environments is also changing, which is causing them to live longer and in different parts of the country where we are not used to seeing them. So Lyme disease is a great example, which increases more exposure and disease outbreaks. And then we also think about extreme weather events, not only the direct trauma, but the disruption to health care systems and to the longer term disruptions and mental health impacts. And then there’s the social implications of being displaced from your home. Now that’s just a wide overview, but I think all of that’s to say that there is enormous evidence right now that climate change harms health. We need more information and evidence to understand that in order to guide our response forward. [00:11:09][164.5]
Bill Loveless: [00:11:10] Right. And you’ve written about environmental justice issues as well. Tell us about the maybe the story you told about the young girl with asthma. I think there was also there was sort of the environmental justice aspect of that story, too. Am I right? [00:11:24][13.8]
Renee Salas: [00:11:25] Yeah, I health, actually. And social justice are critical underpinnings of climate change because we cannot achieve those without action on climate change. So I view climate action as a prescription for improved health and equity. So climate change not only creates new health inequities, but worsens existing ones. Oftentimes, I think about climate change as a threat multiplier, just meaning that it’s worsening existing issues. So another example is historical redlining again outlawed now, but it led to blacks living in certain parts of cities that have been found to now, even today be sometimes upwards of 20 degrees Fahrenheit hotter than other areas in the community. Now that is another example of how climate change is worsening these existing inequities. And it is critically important for us to identify that and make sure we can prioritize resources there. [00:12:31][65.9]
Bill Loveless: [00:12:32] For what kind of attention is this getting in the medical community now are many doctors applying what you call a climate lens to the diagnosis and treatment decisions? [00:12:41][9.6]
Renee Salas: [00:12:43] Yeah, I’m a I’m a photographer. I have not as much done. I have not done that as much recently due to obviously other efforts. But I think that that for me just resonates, that we have to look at everything and understand how climate change is impacting it now and how it’s going to impact it in the future, because we cannot optimally prepare for what we don’t fully understand. And so adding a climate lens to everything we do in medicine really shows that climate change threatens the very reasons why we went into health in the first place, which is to improve health, prevent harm and accelerate equity. And the medical community is a sleeping giant that is awakening around this issue. It’s seen that it is fundamental for us to engage on this upstream and downstream in order to implement adaptation if we actually want to achieve our goals. And so that is involved. The National Academy of Medicine having a big effort. The New England Journal of Medicine, which is a leading medical journal in addition to The Lancet, which has been long engaged, is stepping forward and we’re really on the cusp, I think of unprecedented action and movement within the health sector. [00:13:54][71.8]
Bill Loveless: [00:13:55] Yeah, I’ve read where the Center for Climate, Health and Global Environment at Harvard’s T.H. Chan School of Public Health has a program called Climate M.D., which you and Dr. Aaron Bernstein, head. And as I understand it, Climate MD focuses on the health care effects of climate change and aims to prepare a climate ready health care workforce. What is a climate ready health care workforce? [00:14:18][23.1]
Renee Salas: [00:14:20] Yeah, case back to that toolbox that we talked about in the sense that we do not currently ensure that clinicians have the tools they need to operate in a 21st century environment, and that involves a spectrum of things. So I mean, first off, it’s adding a climate lens to medical education to make sure that students and trainees can understand how climate change is really impacting everything it is that they’re learning. And I think educators often struggle and say, Oh my gosh, do I have to add a whole new topic to this? And it’s no. It can be anything from a problem based learning case, having a few learning objectives about how climate change is impacting what they’re studying. And then it’s for clinicians who are already working and practicing. It’s making sure that they understand how climate change is evolving within their area. So as vector borne diseases and for example, Lyme disease, which they had not historically seen, is now emerging into their region, that they can keep that at the forefront, which is the importance of making sure they have the data they need. And then I think that the third thing that I’ll touch on is also recognizing that health, the health care system itself is disrupted because of climate change, and that can be everything from impacting infrastructure to having power outages or not having the supplies we need. And all of that makes it harder for me to do my job in the emergency department, which is to provide the highest quality care I can to the patient in front of me. [00:15:54][93.8]
Bill Loveless: [00:15:54] Well, you say there’s greater attention to this issue now, but you know, when you’re in the emergency room, do you feel as though you have the tools and the means necessary to respond effectively to your patients? [00:16:07][12.4]
Renee Salas: [00:16:08] I think the the COVID 19 pandemic has has shown us how. Our current environment is not equipped for frequent and sustained shocks. And I think that that has been really a wake up call for many people, and those rose colored glasses have been knocked off because that has been happening at the same time that we have really seen climate intensified events filling our headlines and impacting our hospitals. I have colleagues out in the northwest who experience that unprecedented heat wave in June of 2021, which would have been impossible without climate change, according to climate scientists. It was hundred and degrees Fahrenheit in Portland, Oregon, and the stories there of of not being equipped to be able to handle that mass influx of patients. So some emergency departments actually saw visits for heat related illness that was 70 times above what they’d seen in 2019. So the short answer is no, we’re not where we need to be. But I have seen the health system respond quickly in the COVID 19 pandemic, producing the data. We need having that unprecedented collaboration to share innovation, and we can do that again for climate change. [00:17:27][79.4]
Bill Loveless: [00:17:28] Maybe some lessons here that will be learned and proved to be effective in dealing with this going forward. You mentioned Lancet before, and you’ve served as a lead author of the annual Lancet Countdown on Health and Climate Change, which is an international research collaboration that tracks the relationship between health and climate and its implications for national governments. I should mentioned as well among the contributing authors is one of my colleagues at the Center on Global Energy Policy, Melissa Lott, who is the head of research for the center. What are what are the main takeaways of the most recent report? [00:18:06][37.4]
Renee Salas: [00:18:07] Yes, Melissa is wonderful, and the I and I have had the honor and privilege of leading the U.S. brief since 2018. In addition to recently serving on the global report and the take homes are is that it is a code red for health. And I think that as an emergency medicine doctor, that that really resonates, that we are not treating it like the emergency that we need to. And so it is shown that the impacts are growing around the world and the fact that it is not equitably being experienced. And so I think the global report really highlights the fact that certain countries and individuals are disproportionately bearing the brunt, and our U.S. brief furthers that and shows that it is still and equitably being experienced here. But at the same time, the fact that it impacts everyone again, to some degree, I think there were three additional key themes. I’ll just hit quickly on the U.S. brief, and the first is is recognizing that we are all interconnected. And the fact that the the wildfire smoke that was being produced out in the West actually traveled all the way across the country and led to New York City having its worst air quality day in 15 years. So we are truly interconnected. We talk about drought and the fact that the health impacts are really broad and surprising, sometimes in regards to how health can be impacted. And then the last one is is thinking around the heat and extreme heat impacts and how different populations are disproportionately impacted. Again, themes that resonate across other exposures as well. [00:19:51][104.4]
Bill Loveless: [00:19:52] And of course, the report has is intended to inform us all, but also to inform national governments correct. I mean, that’s one of the goals it seeks. Are these concerns getting much attention in policymaking circles in Washington among the states? [00:20:09][17.0]
Renee Salas: [00:20:10] So you’re right, it’s purposely released right before cop. And so this one was meant to influence the discussion at COP 26 and to track the action or inaction that’s occurring. And the U.S. brief also highlights three policy recommendations about how we need to increase adaptation the the health benefits of mitigation because we need to ensure that health not only motivates us on why to act of having improved health, but also guides our response and especially also with equity considerations. And then the financial considerations. And I think that at least those three themes within the U.S. have resonated with policymakers. And I think that there is again, a growing recognition of the importance and the current administration is taking that all of government approach, which has included creating an office within Health and human services. And it is our hope that that health will continue again to serve as that not only motivation for what. We need to act on climate change, but also to guide our response. [00:21:17][66.7]
Bill Loveless: [00:21:18] You know, Gene McCarthy, President Biden’s national climate adviser, launched the Center for Climate, Health and Global Environment, or Harvard Chan SeaChange, as you know, before going to work for the administration. She’s still focusing on this topic. And do you talk to her? [00:21:34][15.3]
Renee Salas: [00:21:34] I’ve had the honor and privilege she has has been a mentor of mine. And so yes, she is at the helm. Within the within the White House of really leading this effort. And I can’t think of anyone better to do it. And she has taught me, as with so many others, the importance of thinking about climate change as a health crisis. But I think, more importantly, recognizing that the health benefits are profound. With climate action [00:22:05][31.0]
Bill Loveless: [00:22:06] and you’ve also you’ve testified in Congress on this topic, including at least once I’ve seen where before a House committee that was was looking at these issues, the House Oversight Committee on Oversight, well, oversight and Reform. How did that experience ago and what did you learn about the way policymakers think and talk about climate change? Hmm. [00:22:29][22.5]
Renee Salas: [00:22:30] I think the health benefits of climate action have been grossly under-recognised, and you brought up before about thinking about the parallels with the COVID 19 pandemic. I mean, I think one of them has to be that we have seen firsthand how health and having optimal health is is fundamental to a thriving and functioning society. And I argue the same is true for climate change. And so. It has been an increasingly recognized connection that I hope that if we can frame climate action through the lens of the health and equity benefits that we can begin to come together and recognize the importance of that. And so I felt that that experience of testifying was really me having that unique opportunity to bring the voices of my patients to the halls of power and to ensure that those voices were heard because we see a lot of climate stats. But it is those narratives, those human narratives that are our sons and daughters that are aging parents that are ourselves or our neighbors, and making sure that we see that we are the faces of climate change. And I can’t think of any bigger motivation to act than that. [00:23:50][79.9]
Bill Loveless: [00:23:50] You mentioned Cop 26, before the the global climate meeting in Glasgow, Scotland, that took place in the fall you attended the COP26. What initiatives did you participate in and how did you see the experience shaping the way you think about crafting climate policy and at a policy scale? That’s that’s necessary? [00:24:16][25.5]
Renee Salas: [00:24:17] Yeah, I had the honor of attending actually both weeks as part of the Harvard delegation, and for me, this was my second cop overall. And it is in so many ways, a really inspiring experience. I mean, I think especially for so many of us that had not actually been together in the same row, we’d been seeing each other on screens as so as so much of our interaction has been during this pandemic. What we were actually in the same room together and seeing people from all over the world come from the health perspective and represent their patients and communities, to me showed that again, we are on the cusp of the the the giant awakening within the medical community because we will not rest until the health of our patients is optimally protected and in climate action is fundamental for that. So I walked away, inspired by and humbled by all of the action going on around the world and how we can learn from each other. Because as we know, just like the one country does or doesn’t do in regards to management of the pandemic, how that affects everyone else. The same is true here with climate change because greenhouse gases don’t respect country borders. And so we are truly all in this together and oftentimes are. We are struck with the differences that we have, and I think that makes the headlines more than what brings us together. But climate change can truly unites us and binds our fates together, which means that we have a common purpose moving forward to act on this. [00:25:54][96.8]
Bill Loveless: [00:25:55] As I hear you talk about the work you’re doing on the policy front and as well as on the education front, in your profession and testimony you’ve done in Washington and participation, you had it at the cop cop meeting and Scotland. You know, I can’t help but ask, did you ever think about stepping aside from your clinical practice to it to concentrate on this bigger issue and perhaps a bigger way? [00:26:16][21.7]
Renee Salas: [00:26:17] Well, I I have continued to step away in and I am now at the point where I work the least amount that our department allows because I do feel that my calling really is, is this work? And I don’t know what the future holds, but we do have a forthcoming, ambitious endeavor that may, may require me to step out of the walls of the emergency department, at least for a bit. But right now, I think it still gives me so much joy to see patients and and to see the reason it is I’m doing all of the work upstream. [00:26:53][35.9]
Bill Loveless: [00:26:54] You know, our discussion comes just just a few days after the death of Dr. Paul Farmer, a graduate of Harvard Medical School and who’s so well known for his work promoting health as as a human right in Haiti, Rwanda. What does he and his work mean to you as as you look to make changes and approaches to medicine? [00:27:14][19.9]
Renee Salas: [00:27:15] Yeah, I actually had the honor and privilege of joining his department at the medical school recently, and he clearly saw that action on climate change was central to everything it was that he stood for and around health equity and social justice. And there’s a quote that. He said that has been circulating since his untimely passing, and that was the idea that some lives matter less is the root of all that’s wrong with the world. And I think for so many, these big interconnected challenges like climate change can seem overwhelming, but we really recognize that it’s all interconnected and if we can put. Our love for one another and our health and humans at the center of this and again have those health and equity benefits guide our path forward for climate change. We can really tackle so many of the other interconnected problems because these interconnected challenges mean they have interconnected solutions so we can rise above multiple challenges at once. So whether we’re trying to prepare our hospitals to be more resilient to the next pandemic or the next climate intensified exposure threat, all of that is intertwined. And I think that there is an enormous responsibility for us to continue his legacy and honor that through the work. And I can’t think of a bigger way to do that than through acting on climate change in the way that it needs to to put health equity and social justice first. [00:28:52][97.2]
Bill Loveless: [00:28:53] You know, you seem somewhat optimistic. Maybe I shouldn’t say somewhat but optimistic that this this need to connect climate and health. The impact on people’s, you know, very health day in and day out is this is getting increasing attention in schools and and all. And even, you know, in Washington and you say in the administration and even among lawmakers up on Capitol Hill, what is it that you may concern you most about what isn’t getting sufficient attention here or sufficient action? [00:29:26][33.7]
Renee Salas: [00:29:28] Well, we are at the at the cusp. I think of that exponential understanding. So we are there’s growing understanding, but we still have significant gains that need to be made. But the ground has shifted so much within the past, I would argue, even one or two years. And. The COVID 19 pandemic has again shown us how underprepared we are in so many ways, but it’s also provided us an opportunity in this accelerated experience to see what the implications are for longer term problems like climate change that have been unfolding under our eyes. And I, I am enormously optimistic because we have everything we need to act, and I think you and your colleagues know more than than any of us in regards to how quickly and equitably different possibilities can be implemented around renewable energy sources and healthy. I would argue healthy energy sources if we’re going to frame this from a health standpoint. And so we have the tools we need. We just need the will [00:30:41][72.8]
Bill Loveless: [00:30:41] and the will is certainly there with you and as you say, among many of your colleagues in the in the medical community. Dr. Rene Solis, thanks for joining us on Columbia Energy Exchange and discussing this important topic. [00:30:54][13.0]
Renee Salas: [00:30:55] Thank you. It’s an honor, a privilege to be here and thank you for bringing the health lens to climate change on your podcast. [00:31:01][5.8]
Bill Loveless: [00:31:05] Thank you again, Renee Salas, and thank you for joining us on Columbia Energy Exchange. The show is brought to you by the Center on Global Energy Policy at Columbia University’s School of International and Public Affairs. The show is hosted by Jason Bordoff and Me Bill Loveless. The show is produced by Steven Lacy, Jaime Keizer and Alexandria. Her from PostScript Audio. Additional support from Tori Lavelle, Kristin Smith, Daniel Prop, Natalie Volk and Q Lee. Sean Marquand is our sound engineer. For more information about the podcast or the Center on Global Energy Policy, visit us online at energy policy that Columbia Dot Edu. Or follow us on social media at Columbia. You energy and if you can, please give us a five star rating on Apple Podcasts. It helps the show reach more listeners like you. We’ll see you next week. [00:31:05][0.0]
More Episodes
Alex Fitzsimmons on the DOE’s ‘Energy Dominance’ Agenda
Under the second Trump administration, the US Department of Energy significantly shifted its priorities to align with its “energy dominance" agenda. But one significant point of continuity with...

Laura Holgate on the Promise and Perils of Nuclear Innovation
The Trump administration has prioritized nuclear energy expansion, aiming to increase US nuclear capacity fourfold by 2050. This nuclear energy resurgence in the US is a rare issue...

Jigar Shah Wants to Depoliticize Energy
As political support for clean energy has waxed and waned over the past twenty years, so has the government’s financial backing. In the 2010s, critics pointed to the...

Michael Webber on What’s Behind Rising Energy Costs
With electricity prices on the rise, the future of our power grid is attracting a lot more attention. Surging demand is at the center of the story, but...

Relevant
Publications
The Climate Question That Economists Cannot Answer
Models can predict catastrophic or modest damages from climate change, but not which of these futures is coming.

Regulatory Progress for Project-Based Carbon Credit Markets: Pre-COP30 Roundtable Summary
On November 6, 2025, in the lead-up to the annual UN Conference of the Parties (COP30), the Center on Global Energy Policy (CGEP) at Columbia University SIPA convened a roundtable on project-based carbon credit markets (PCCMs) in São Paulo, Brazil—a country that both hosted this year’s COP and is well-positioned to shape the next phase of global carbon markets by leveraging its experience in nature-based solutions.

Opinion: Time for CT to rethink its climate strategy
Connecticut needs an honest debate, and fresh thinking, to shape a climate strategy fit for today, not 2022.
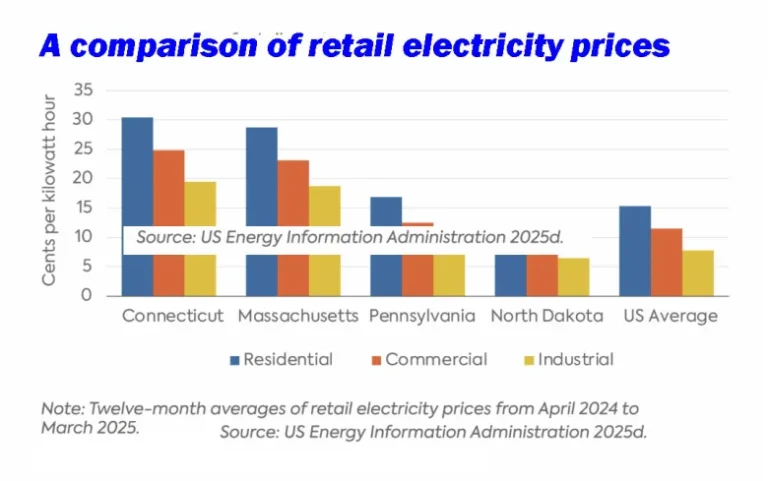
Climate Ambition and Electricity Affordability: Lessons from Connecticut


